THE SKIN AND THE SUN
Luciano Schiazza M.D.
Dermatologist
c/o InMedica - Centro Medico Polispecialistico
Largo XII Ottobre 62
cell 335.655.97.70 - office 010 5701818
www.lucianoschiazza.it
Man has always associated sunlight with physical health, cult, adoration. From the Egyptian God of Sun (RA), to the Greek Apollus (God of Light and Wisdom), to the Aztec God of Sun (Tonatiuth), the symbol of the sun, representing authority and majesty, has characterised the history of numerous civilisations throughout the centuries. Not to forget the authoritarian association with sunlight that Louis XIV evoked for his reign (the King of the Sun).
Nowadays, all this has been transferred to an individual level and the cult and adoration of the sun has turned into a fashion phenomenon: bronzed skin is identified with health, wellness, distinction and social prestige. The suntan has taken on symbolic aspects: for many of us it is a goal, an ambition to comply with social models based on images of success, youth and seduction.
This false idea of physical beauty has induced and induces people to try and maintain an ambered skin all year round, despite the repeated admonishments and warnings of dermatologists against this behaviour.
At this point, in order to clarify the relationship between sunlight and skin, it will be necessary to define the physical and biological characteristics of sun rays, the role and the meaning of melanogenesis, the constitutional traits of individuals, the properties of the products that provide protection against sun rays when applied to the skin.
SOLAR RADIATIONS
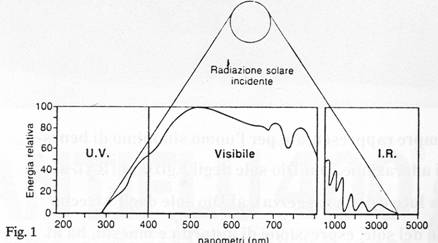
The energy produced by the sun is transmitted through electromagnetic radiations. The solar spectrum reaching the earths surface (fig. 1) accounts for a small portion of the energy produced by the sun (fig. 2): this happens as a result of the atmosphere and in particular of the ozone layer (O3) in the stratosphere. This essential photoprotective agent basically acts as a filter, absorbing radiations below 285 nm (nm=nanometre: is conventionally adopted as measure unit for solar radiations and corresponds to 10-9 meters, equivalent to a millimicron, that is a millionth millimetre). It is found between 15 and above sea level and forms as a result of the reaction with specific ultraviolet rays (UVR), UVC: (fig. 3) when UVC strike an oxygen molecule (O2), they split the molecule into two single oxygen atoms (O+O=2O), which rapidly combine with other intact oxygen molecules (O2) thus forming ozone (O3).
O2 ---uv-c----------- 2O |
2O + 2O2----------- 2O3 |
As a result of its ability to absorb ultraviolet light easily, this gas is again split into the two components (O2 and O) , in a continuous sequence of dissociation and formation. This determines a status of static equality between the two processes resulting, under steady conditions, in ozone stabilization.
Ozone blocks various radiations (harmful to living beings) with a very strong absorption band between 200 and 310 nm (Halery band) and a weaker one between 310 and 350 nm (Huggins band). In particular, ozone blocks UVC, high energy short ultraviolet rays (190-290 nm), and very short wavelength radiations (X rays, gamma rays and cosmic rays); if these rays were not screened, they would prevent any form of animal life, due to their ability to penetrate deeply into tissues.
The ozone layer width is not uniform but it varies according to the latitude reaching its minimum at the equator and its maximum in the polar regions, with seasonal variations at medium latitudes where it is maximum at the beginning of spring and minimum towards the end of autumn; seasonal variations are minimal in the tropical areas.
The intensity of UV rays reaching the earth depends on various factors: latitude, time of exposure, altitude, atmospheric humidity, type of soil surface.
The energy of radiations on the earth is inversely proportional to their path in the atmosphere: therefore the shorter the path the greater their energy. At >midday when the sun is perpendicular to the earth’s surface (zenith), the risks of erythema are higher than at 5 pm , when solar rays are more oblique and pass through a thicker ozone layer.
The radiation path is also reduced at higher altitudes, the atmosphere is less turbid and the mass of the air to pass through is smaller: hence there is an increase by approximately 15% per 1000 meters above sea level.
Moreover, the lower the atmospheric humidity the greater the transparency to solar radiations: this is particularly evident in the mountains where absolute humidity is lower than that at sea level (at an altitude of 3000 meters it is 1/3 of the one measured at sea level).
One should not forget the effect of reflected solar radiations, which add to direct irradiation: the albedo of a horizontal surface is defined as the relationship between the energy reflected by a surface and the incident energy, that is its percentage reflection ability: thus the snow reflects 84% of it, the sand 17%, a green meadow 3%, water approximately 5% with a maximum of 10% if the sea bed is sandy.
A cloudy sky is not to be underestimated: clouds intensely absorb infrared rays, thus eliminating the sensation of heat, but let considerable shares of UV rays pass through.
CUTANEOUS PHOTOBIOLOGY
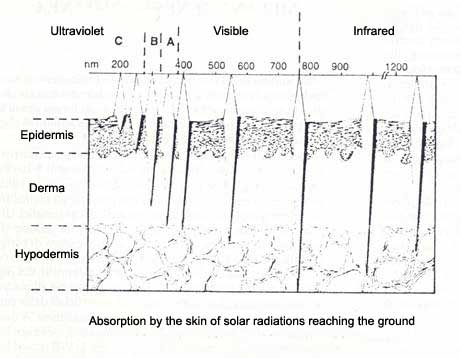
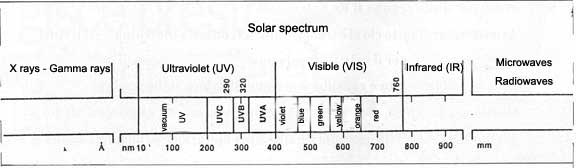
Photobiological dermatological studies (medical studies involving the physiological and pathological changes which the absorption of light causes on the skin) give particular attention to wave lengths between 290 and 800 nm. (fig. 3).
The radiations between 190 e 400 nm. are called ultraviolet rays (UV), even though they are not visible to the human eye. These include:
UVC (short UV: 190-290 nm.): these are dangerous for man, but fortunately are absorbed by the ozone layer.
UVB (medium& UV: 290-320 nm.): represent only 1% of solar radiation reaching the earth. Blocked by glass, 90% of the rays are absorbed by the skin (above all at the corneous level, 80%) while the remaining 10% reach the derma. These rays are responsible for solar erythema (1st degree burning) which manifests itself after about 6-8 hours of sun exposure, reaching the maximum discomfort in the following 12-24 hours and then calming down within a couple of days. They are also responsible for indirect pigmentation due to the activation of a biochemical chain reaction of the melanocytes (see melanogenesis). This appears after about 48-72 hours of exposal to sunlight and reaches its maximum after 2-3 weeks. It lasts a long period of time (weeks or months) and produces a “real” suntan. The UVB, more energetic than the UVA, as a long term effect (years), can also expose us to the risk of photocarcinogenesis, the appearance of skin tumours, following photochemical processes inducing somatic mutations. The development of skin tumours is also favoured by the alteration of the skins immune system, in an immunosuppressive sense, which the UV are capable of inducing.
UVA (long UV: 320-400 nm.): are subdivided into short UVA, whose biological effects are closer to UVB, and long UVA. They can pass through glass and provoke immediate light pigmentation, so called direct pigmentation, whose degree of suntan depends on skin type, previous suntans and the length of exposure. The tan will be more intense in dark skinned subjects and greater depending on the suntan already present. This suntan is very rapid to appear but it is equally rapid in fading away, especially after brief exposures; it could however last more than one and a half days if exposure to high intensity UVA were prolonged. This pigmentation does not have any photoprotective action and will never bring a lasting suntan, as there is no production of new melanin, nor the increased transfer of melanosomes in the keratinocytes.
UVA also have an erythematous effect but in a lesser measure than UVB (in order to obtain the same erythematous effect obtained at 297 nm., one would need one thousand times more irradiative energy at 365 nm.). However, since in the solar spectrum there are more UVA than UVB rays, it is believed that UVA contribute about 15% to the erythematous effect that may be manifested during midday sun. Since the quantity of UVA rays reaching the earth are about 10 times as large as UVB , the cumulative long term effects of UVA radiations can be as important as those of UVB ones, considering also that UVA of superior wave length (over 340 nm.) can have a mutagenic effect and therefore can be carcinogenous, probably due to the synergic action with UVB.
Both UVB and UVA are absorbed by the atmosphere in a directly proportional measure to the thickness of the atmosphere (at the equator the atmospheric layers are more subtle than in the other parts of the globe), to the hydrometric degree (the lower the atmospheric humidity, the greater the quantity of rays that can reach us), to the incidence of rays (the more they are oblique, the longer they will remain in the atmosphere). UVB rays, at our latitudes are practically absent before ten in the morning and after three in the afternoon, whereas they reach their maximum quantity when the sun is at zenith, at midday.) Also, in altitude the quantities of UVA and UVB are very important (4% increase of the intensity for every 300 metres of height) and the phenomenon of reflection of the UV sums with the direct UV in their action on the skin (on the snow the degree of reflection is 0.85, on dry sand it is 0.17, on water it is 0.05).
The radiations of a wavelength between 400 and 800 nm. are indicated with the portion visible in the electromagnetic spectrum or simply with light, to describe a radiation that one visibly perceives (these radiations and in particular those between 420 – 470 nm. are used in the cure of the newborn icterus – phototherapy).
The radiations over 800 nm. (infrared, microwaves and others) do not cause biological effects unless they are not at a sufficient intensity to generate heat and give way to histolesive phenomena.
SKIN MELANOGENESIS
A fundamental role in photoprotection is played by the “epidermal melanin unit a functional and structural unit made up of two cell types: the melanocyte which is a cell in a ramified form specialised in pigment synthesis (melanin) and a bunch of keratinocytes, surrounding the melanocyte, which receive the pigment (36 per each melanocyte)
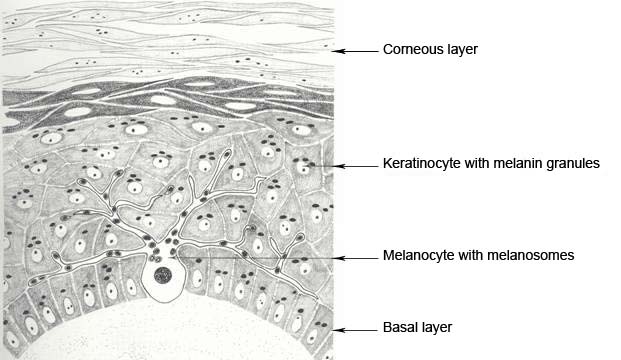
The melanocytes are situated at the level of the germinative layer of the epidermis in the relationship ¼-1/10 (or rather one melanocyte for every 4-10 basal keratinocytes) and put together they would not be larger than a cube of sugar of the volume of 1-1.5 centimetres cubed.
When the UV rays (in particular UVB) reach the skin, there is an increase in the number of functional melanocytes and in the quantity of melanin produced. In particular, inside melanocytes some elliptic-shaped cytoplasmic organelles called melanosomes are present, where the biochemical reaction leading to pigment synthesis (melanin, proteic macromolecule) takes place. As a result of the stimulation by UVB rays, melanosomes are produced in increased quantities and transferred more rapidly through the ramifications, known as dendritic processes (which further increase their size and ramifications), to keratinocytes and afterwards these are dispersed in the skin. The visible result of this process is a suntan. It is important to underline that this is what we mean by a real suntan, as it is a result of melanogenesis, induced by the UVB (the so called indirect or delayed pigmentation).
The pigmentation manifesting itself after exposal to the UVA is defined as direct or immediate pigmentation (IPD = Immediate Pigment Darkening or rather the immediate darkening of the pigment) or the Meirowski phenomenon. This is a fleeting suntan, of a brief duration and the result of a simple oxidative reaction on the melanins present in the still uncoloured superficial skin layers: it is only a superficial phenomenon and cannot sufficiently protect from further sun exposals, as the pigment production is missing. Exposal to UVA sunlamps therefore determines an ephemeral suntan that requires continued exposure to be maintained and this causes other problems in as much as UVA rays are not innocuous: they penetrate the skin deeper than the UVB ones, reaching the derma (fig. 3) where they release their energy, producing irreversible damage to important and delicate structures such as collagen and elastin (dermatoeliosis or photoaging). This happens when solar exposure is chronic and prolonged, as the damaging effects of solar radiations are cumulative and not completely repairable, partly as a result of a direct action and partly related to the formation of free radicals, and collect together on the epidermis and on the derma since childhood. Typical localisations are the regions exposed on the face, on the back of the neck, on the palms of the hands, on the balding head of men and on areas of women’s décolleté. Clinical expressions of photoaging are solar elastosis, cutis romboidalis nuchae (typical of the rear part of the neck that is very wrinkled in people working outdoors like farmers and fishermen), facial teleangectasis, senile lentigo, actynic keratosis, guttate hypermelanosis on the limbs (particularly the front surface of the legs), pigmentations diffused in spots on the back of the hands and on the arms.
As already mentioned, the final product of melanogenesis is melanin. Two types may be distinguished: eumelanin (of a brown black colour, high molecular weight, polymeric structure, insoluble in common solvents) and feomelanin (yellow red colour, soluble in diluted basis, traceable in urine). Eumelanin is present in the Caucasian and Negroid races, therefore in subjects with dark skin and dark hair whereas feomelanin is typical in the Celtic race, with pale skin, numerous freckles and auburn or carrot coloured hair.
This diversity has a determining practical effect on the different protective abilities of the two melanins in defence of UV radiations. In fact feomelanosomes, smaller than melanosomes in the Caucasian race, are transferred in groups to keratinocytes and are rapidly digested in the first layer above the basal layer, thus rendering their protective ability of little significance. In the Caucasian race the small volumed melanosomes are transferred to keratinocytes in packets and they degrade more slowly, but are not found in the corneous layer.
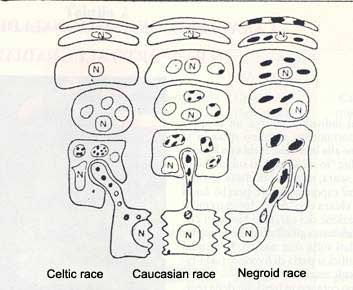
In the Negroid race the melanosomes, apart from being larger and more mature in higher quantities, are transferred as units to keratinocytes and are not digestible, and therefore do not degrade. They are found intact also in the superficial area of the skin (corneous) forming a continuous layer absorbing the UV rays. This different destiny clearly expresses the types of pigmentation of the races indicated in the illustration.
Once the transfer of melanosomes from the melanocytes to the keratinocytes has occurred, these group together under the form of a cap over the nucleus (capping phenomenon) protecting the genetic material of the cell.
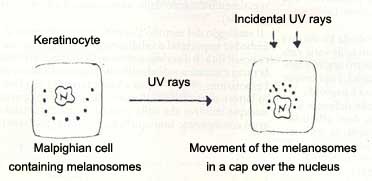
The eumelanin, apart from acting as a filter and as a screen that diffracts and reflects a part of the incidental rays, has a stable “trap” like structure for the free radicals that are formed following exposure to UV radiations. The feomelanins on the other hand increase the production of free radicals demonstrating to be not only without photoprotective activities but real chemical aggressors, thus explaining the photosensibility and the increased carcinogenesis in feomelanitic subjects.
In order to defend itself from ultraviolet irradiation the skin does not only activate melanogenesis but it also starts another process whereby, through the multiplication of layers of keratinocytes, its thickness increases, in a matter of days, practically doubling it. This important form of protection however rapidly disappears after a holiday in the sun and in this way one risks to believe oneself sufficiently protected for further exposals, based on the colour of one’s suntan, not being able to materially verify the thickness of the skin. The same thing happens when one gets an artificial suntan: the melanogenesis does not become stimulated and the epidermis does not become thicker.
The third photoprotective element is represented by urocanic acid (UCA) present in the skin and in sweat. Metabolite of histidine, it increases with solar rays under the action of UVB, in the cis form, to return once again to the trans form in the absence of light. With its filter action energy is dissipated in heat.
Let us not forget a permanent protective screen: body hairs and hair.
CONSTITUTIONAL TRAITS OF THE HUMAN SKIN IN RELATION TO SOLAR RAYS
Each individual reveals its own skin behaviour when exposed to solar light: who has not heard “I get tanned straightaway because I have dark skin; I get sun burnt each time I am exposed to the sun because I have pale skin”. These are two extremes of evaluation of the biological traits that condition the effects of solar radiation on the human skin. In scientific terms, one speaks of phototype or rather the skin biotype in relation to light.
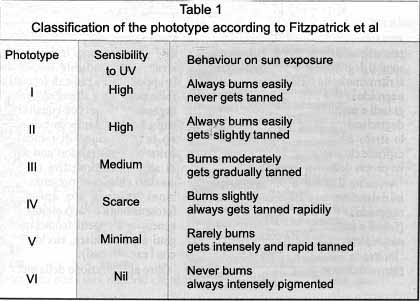
A dermatologist from Boston<, USA, TB. Fitzpatrick, dealt with this matter with scientific rigour, defining skin types in relation to their behaviour during sun exposure. This methodology is based on a solar case history defining the intensity and the duration of the erythematose reaction (burning) and the pigmentation ability (suntan) analysed on the basis of the first 45 – 60 minutes of sun exposure after the winter or after no previous sun exposure.
As one can see in table 1 there are six types of individual skin in the various human races: the first four belong to Caucasian individuals, types five and six belong to hybrid and Negroid subjects and at the extremes are found those individuals who always burn and never get suntanned, while on the other hand are found those who minimally get burned and that always get tanned easily, excluding the phototype VI.
Together with this method, defining the skin type on the basis of the immediate effects of radiation, there are others, in particular the one of Jean Pierre Cesarini who, apart from the solar case history, assumes some phenotypical traits as further parameters for evaluation.
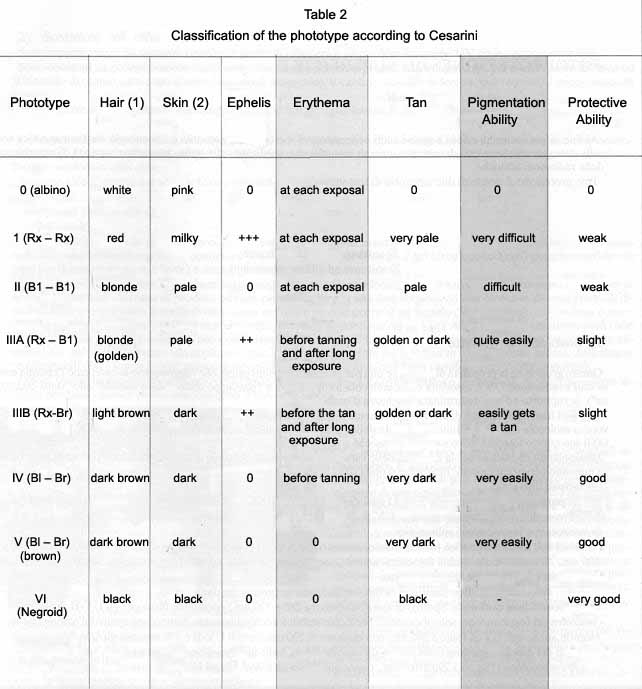
This classification (tab. 2) uses some static elements (hair colour, winter colour of skin, presence of freckles on the areas exposed to the sun – face, shoulders, arms, legs, back) and dynamic elements (lack of erythema, erythema during the first exposure, erythema at each exposure, type of tan).
This author affirms that the base colour of the skin derives from a contribution of three simple traits – red, blonde and brown (hereditary or genetically controlled) whose combinations give way to six possible couplings corresponding to an equal number of phenotypes. On the extremes we find on one side albinos, incapable of synthesizing pigment and therefore without any form of protection if not the thickening of the corneous, and on the other those who are doted with an absolute protection.
SUPERFICIAL PHOTOPROTECTION
With the aim of preventing acute erythematogenous and chronic degenerative effects of electromagnetic solar energy on the skin, one should use substances that on application to the skin assure the ability of blocking the actinic radiations totally or partially.
This protection consists of two substantial categories:
-
Substances with a filtering effect
-
Substances with a screening effect
Substances with a filtering effect (chemical filters)
This group includes compositions that partially absorb a portion of radiations before they reach the skin: the energy released by UV radiations is absorbed by the photoprotective molecule (path from the “initial state” to the “state of excitement”) in relation to a determined wave length.
These filters have the ability of slowly liberating the energy absorbed in the form of heat or fluorescence with a return to the state of non excitement or to remain stable in their “excited state”. They offer therefore a protection against the sun that is potentially maintained for a long time.
The chemical manipulation of the various molecular structures has enabled the diversification of their power of absorption towards determined wave lengths in respect of the spectrum: in the formulation of a sun screen this has imposed the use of different substances in order to reach a complete protection.
The main filters are:
PABA ( para-amino-benzoic acid) and derivates
PABA is partially active on UVB, hardly at all on UVA. Insoluble in water, it can cause an allergy combined with the so called “para derivates” (thiazidic diuretics, local anaesthetics, sulphamides). This was used particularly in the 50’s and the 60’s, in the present day derivates are preferred, many of which are water soluble and do not penetrate the skin, reducing in this way the risks of contact dermatitis or photosensibilization. The PABA derivates partially protect from UVB whilst they are inactive against UVA.
Derivates from cinnamic acid (cinnamates)
They have a spectrum of action with maximum absorption of the UVB, with a peak of maximum absorption ability of around 310 nm., but at 340 nm. they still manage to protect from 40% of UVA. They have little substantivity and this makes them not very water resistant. They are frequently used for their low cost and their scarce ability of penetrating in the corneous layer which makes them practically atoxic. They are generally used in combination with other photoprotective substances.
Salicylates
They offer little photoprotection, but are often used because they are stable, not sensibilizing and insoluble in water, thus allowing use in water resistant products, atoxic and relatively cheap. They are furthermore used in formulating a sun protection product, to solubilize other products that are scarcely soluble. Their spectrum of action is only relevant to UVB with a maximum level of absorption of around 300 nm.
Benzophenones
Photochemically stable molecules, their spectrum of action regards above all UVA (320-350 nm).
Dibenzoylmethane
These composites offer an optimal absorption ability of UVB and UVA, having a spectrum of action between 290 and 370 nm.; nonetheless their instability determines, under the action of light, the production of other composites with different physical properties that are not equally efficient.
Substances with screening effect (physical filters)
They are represented by heavy metal particles able to disperse, reflect or absorb both UV rays and visible radiations. They are made up of white powders with high covering power. Amongst the most frequently used are zinc oxide, titanium bioxide, iron oxide, caolin. At the beginning their use presented limits (comedogenicity, photosensibility, photodegradability, the white mask like appearance on the skin after product application) but thanks to recent technology and micronization techniques it has been possible to obtain very fine powders that are cosmetically acceptable, invisible on the skin, stable, non photosensibilizing, consenting therefore to overcome the previous limits.
Such substances are used in the photoprotection of subjects particularly sensitive to UV: not only those who are sensitive due to their phototype, but also and above all, for those people who are affected by dermatosis, developing cutaneous eruptions after exposal to UVB, UVA and/or visible light. An example is the polymorphic eruption to the light, solar rash, the lupus erythematosus, dermatomyositis, pigmented xeroderma.
Today, research conducted by many cosmetics companies has allowed an effective improvement of filters, of skin tolerance and has ensured uniform coverage over the whole UVA-UVB spectrum. Moreover, active principles have been added that strengthen the physiological protective skin properties, neutralising the affects of free radicals produced by sun exposure.
The formulation of a sun protection product today makes use of an association of one or more filters and/or screens, each one in a modest quantity in order to ensure safety of use in terms of photoprotection and in terms of reduced absorption. To this one adds the use of selected vehicles or excipients that carry out an essential role for the efficiency of the product and for its even distribution on the skin. They are available in various formulations: emulsions, milk, cream, spray, lotion, gel, stick and their use can be adapted to skin type, use needs and acceptance from a cosmetic point of view.
The sun protection factor (SPF = Sun Protector Factor), indicated on the packaging with a number refers to the ability of the product to filter or screen UVB sun rays which induce erythema (the higher the number the greater is the protection factor). This does not include UVA, apparently lighter and more innocuous but in reality more penetrating into the skin and responsible not only for premature aging but also for dark spots, and phototoxic and photoallergic reactions. For the UVA there would be other methods such as IPD (Immediate Pigment Darkening) and PPD (Persistent Pigment Darkening), which however have their limits in reproductionability, definitely better in the latter case.
This factor is calculated, with a static test, comparing the quantity of time necessary to produce a minimal erythema (MED, minimal erythema dose) on skin protected by sun filters compared with the time necessary to cause an erythema on unprotected skin. If for example a person with pale skin were to manifest an erythema after a ten minute exposure, using a sun screen with SPF 15, 150 minutes of exposure would be required (10 x 15 = 150) before becoming red. The degree of protection does not increase in proportion to the SPF. With a factor of 30, 97% of the erythematogenous rays are absorbed, while with a SPF15 the percentage goes down to 93% and with SPF2 it goes down to 50%. Were the product to protect also against UVA, then this would be indicated on the packaging.
Today the manufacturers use the COLIPA method as a reference procedure for the assessment of the photoprotection index, corresponding to the European Cosmetic Toiletry and Perfumery Association, which guarantees the best parameters of standardization and reproductionability thanks, above all, to the optimization of the characteristics of the source of irradiation and the reading of the MED with colorimetric instruments.
In practical terms, however, the protection received can be different to the protection indicated by the label. This is because rarely the same amount of product would be applied to the skin as it is applied in the laboratory (2 mg. per cm2): an adult subject should apply 40 grams each time in order to protect all the exposed areas of his body and comply with the SPF factor indicated on the packaging. Moreover very often one forgets to re-apply the sun protection product after the first application or does it without respecting the recommended intervals (usually every 2 hours or after swimming or heavy sweating). Among the other factors, which may influence the effectiveness of solar screens in everyday life, one must not forget the time between application and exposure (at least 30 minutes) , the effect of external solar light, which during comparison tests with a laboratory solar simulator tends to give lower SPF values, the composition of the formulation, the persistency (the screen ability to preserve its effectiveness upon normal use) and the substantivity (the ability of the screen to remain in the superficial layers of the skin after application) of the product, important above all in order to ensure product effectiveness even after heavy sweating and bathing. With regards to bathing, let us not forget that sea water removes a lower amount of filter than the water of a lake, a river or a swimming pool and that a higher water temperature reduces the duration of the protection.
It is useful to underline that the use of solar screens does not aim to prolong the time spent under the sun: in this way we would substitute the protection from acute to chronic radiation. They help to protect the skin during normal exposure.
Regarding the possible negative effects of solar screens on the synthesis of vitamin D3, in particular in the child and in the elderly, casual exposure to solar light guarantees the maintenance of an adequate state of this vitamin. In fact, UVB rays which pass through thin clothing and hit not adequately protected skin regions allow the organism to get the necessary daily requirements of vitamin D3. In the elderly, who have not suffered from considerable damage due to sun light exposure, only frequent and short periods of face and upper limbs exposure are recommended; it would be enough to be exposed to the sun for 15 minutes 2-3 times a week between the hours 11 and 14 during the summer period or having a total body exposure for 30 minutes a week to cover the minimum needs of the vitamin. In the milking baby two hours a week of head and hands exposure would be sufficient. In the case of subjects that need to use total filters one could suggest an increase of vitamin D3 assumed with the diet (200 UD/day contained in a pill or in 3 glasses of milk).
ADVICE FOR BETTER SUN EXPOSURE
-
Expose yourself to the sun gradually, especially in the first days, alternating sun and shade, to allow the skin to get used to the sun. The paler the skin the more slowly the exposure time should be increased.
-
Use a total sun block. Initially with a SPF of 15 upwards to protect from burning. After this adapt it to your phototype and the place in which you are exposed.
-
Apply the sun screen 30 to 60 minutes before sun exposure and in a generous manner.
-
Apply the sun screen evenly: it may be useful to apply the product in two consecutive applications.
-
Apply the sun block at least every two hours and always after a swim or after having sweated heavily.
-
Don’t forget to protect the ears helix, the rear of the neck, the bald part of the head, the superior part of the foot including the toes, behind the knees.
-
At a high altitude, if you practice mountaineering or skiing, the risk of burning is even greater so always use high SPF screens, not forgetting to apply it on the nose, ears and lips
-
At the equator the sun is stronger. Use filters of 15 and up.
-
If the sky is cloudy, do not forget to apply a sun screen: 80% of the rays pass through the clouds and reach our skin.
-
Under the beach umbrella protect yourself all the same: staying in the shade is a help but does not protect from reflected or diffused rays.
-
Reduce solar exposure to a minimum between 11 and 16 (legal time), hours in which the rays are at maximum. Plan activities in the open air during the first part of the morning and in the later afternoon. Remember that one should not expose oneself to the sun when the shadow is shorter than the height of the object that has generated it.
-
Attention to reflecting surfaces. Sand, snow, ice, concrete surfaces can reflect up to 80% of solar rays on our skin.
-
Protect children. If they are under six months they should totally avoid sun exposal. After this, teach them as early as possible how to protect themselves from the sun. The damage is done as of the first exposure and accumulates during the course of life. It has been calculated that 80% of sun exposure in life happens in the first 18 years of life. Protect them therefore with a suitable sun block and hat, shirt and sunglasses.
-
Be careful with medicines. Some medicines can increase sun sensitivity. If you are using medicine, before exposing yourself to the sun always ask your doctor or pharmacist.
-
Try to avoid staying for a long time immobile under the sun. It is better to move around, rather than lying down, and also in this case change positions frequently.
-
Always use sunglasses. The eyes can also suffer from the damage of ultraviolet light. Protect them with good quality lenses that are able to screen UV rays.
-
Attention to the wind. The freshness of the wind on the skin may lead to incautiously prolonging the exposure times with greater risks of burning.
-
Never use perfumes or scented deodorants when exposing yourself to the sun: in this way one can avoid getting spots on the skin.
-
Avoid the use of reflecting surfaces to increase the suntan.
-
Warning: the burning caused by an excessive exposal to the sun may not be fully visible straightaway, and may only become fully visible after 24 hours.
-
In the evening after the shower apply an after sun cream on the skin of the face and the body.

