Versione Italiana
HERPES GENITALIS
If you know it, you can defend yourself
Luciano Schiazza M.D.
Dermatologist
c/o InMedica - Centro Medico Polispecialistico
Largo XII Ottobre 62
cell 335.655.97.70 - office 010 5701818
www.lucianoschiazza.it
INTRODUCTION
Genital herpes is one of the most common sexually transmissible diseases.
It is caused by a virus, Herpes Simplex Virus (HSV).
There are two kinds of HSV:
HSV-1 that generally is associated with infection of the upper part of the body (mouth and face) (e.g. mouth herpes) HSV- 2 that mainly causes infection in the lower part of the body (mainly in the genital region).
Only in the USA 45 million, mostly women, are infected.
The infection is not life threatening for the patient, however, the risk of infection in the fetus is much greater if a pregnant woman develops her first episode of genital herpes late in pregnancy.
Genital herpes might have a significant impact in patients’ life, not only for the transmission of the virus, but also for the possibility to simultaneously transmit and get infected with other sexually transmissible diseases, including HIV.
The diffusion of the virus is increasing: this comes from the fact that most of the people infected are not aware of it. Moreover they don’t know that the virus is periodically shed.
In fact, only 20% of the infected patients have clear symptoms easy to diagnose, while the remaining 80% have light symptoms (undiagnosed) or asymptomatic disease.
It is therefore important that all sexually active people are aware of the possibility to get infected with genital herpes.
REMEMBER
Learn how to know, deal with it and defend yourself
WHAT IS GENITAL HERPES
Genital herpes is a viral disease transmitted during sexual intercourses: vaginal, anal and oral.
Genital herpes is a sexually transmitted disease (STD) caused by the herpes simplex viruses type 1 (HSV-1) and type 2 (HSV-2).
Genital herpes is mostly caused by HSV-2 (90%). However, nowadays there is an increased number of people infected with HSV-1 in the genital area, due to oro-genital and anal intercourses.
Transmission is always inter-human and infection comes from sexual intercourses. Indirect transmission is quite impossible because the virus inactivates at room temperature.
The “door” to the virus, favored by alterations of the epithelial tissue, are male and female genital membrane and anal area through which the virus easily penetrates and infects the epithelial cells. Normally the first contact with virus is asymptomatic.
Once in the body the virus will stay forever. In some individuals it manifests occasionally, while some others can have symptoms years after contracting the virus.
SIGNS AND SYMPTOM
Most individuals have no or minimal signs or symptoms from HSV-1 or HSV-2 infection.
Signs and symptoms of a primary episode of genital herpes vary widely, if the first episode comes soon after the contact with HSV (either type 1 or 2) (In this case it is called Primary Genital Herpes), or ,as often happens, it is a recurrence of the infection that stays latent in our body (in this case we talk about Recurrent Genital Herpes).
Primary infection either clinically manifested or not, determines an immune response that develops anti-bodies against HSV; it doesn’t, however, eliminate the virus or fully protect against reinfection or recurrence of the disease. which will stay within the body forever.
In fact, after invading the skin, or mucous membranes, the virus travels the sensory nerves at the end of the spinal cord (spinal ganglia) corresponding to the cutaneous area of contact.
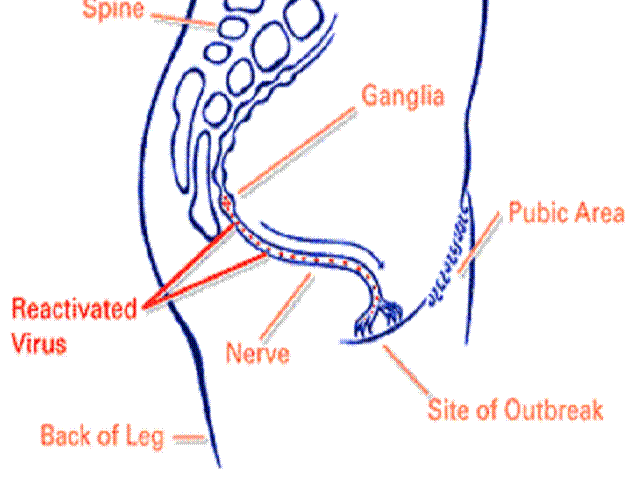
Here the virus will stay forever, inactive, or latent, in perfect balance with the immune defenses of the body. In fact the virus in this situation doesn’t produce viral protein and can’t therefore be detected by host defence mechanisms. Risk factors such as fever, illness or infection, stress, weakened immune system, menstruation, long periods of exposure to sunlight or very cold weather can initiate the recurrence of the infection. These factors trigger the replication of the virus and its “reverse” migration towards mucous membrane. (fig.1)
The possibility to become ill with Primary Genital Herpes is rare, while infected patients are commonly disturbed by recurrent outbreaks (Recurrent Genital Herpes), that according to their frequency, may affect the patient both physically and psychologically.
While in the acute phase of the outbreak the possibility to transmit the virus to the sexual partner is obvious, in the majority of cases (80%) the transmission occurs while the virus is dormant. This is why 20% of people infected with HSV have never had symptoms of the disease, or if they had any, (60%) they went unnoticed. The virus can be eliminated from the mucous membranes in the periods between outbreaks. This is called “asymptomatic viral elimination.
PRIMARY GENITAL HERPES
Primary Genital Herpes occurs rarely and it is particularly severe from the symptomatic point of view (general and local), either with HSV-1 or HSV-2 infection. Primary attack tends to be more severe than recurrent attacks.
The incubation period varies from 2 to 7days. Typically the disease present as multiple, grouped painful genital or peri-genital vesicles on an erythematous base. Rapidly the blisters break, leaving tender ulcers (sores) that may take two to four weeks to heal spontaneously.
Often the skin of the previously affected area is discolored. Cutaneous lesions last about 2-6 weeks. Disuria, enlargement and tenderness of regional lymph nodes may occur. Primary genital herpes tends to produce more systemic symptoms (i.e. fever, general malaise, anthralgia, headache).
The above described symptoms can be accompanied by pharyngitis and other complications (due to over bacterial or mycotic infection), extragenital (contagion through the hands to eyes, buttocks, tighs), general (central nervous system), or by dissemination, in patients affected with atopic dermatitis, with the diffusion of the infection to large body areas.
RECURRENT GENITAL HERPES
Typically, another outbreak can appear weeks or months after the first, but it is almost always less severe and shorter than the first outbreak. With recurrent genital herpes antibodies help ensure that recurrent symptoms are milder than the first episode. Fever and the above mentioned symptoms are usually absent and local infection milder.
Itching, burning or tingling in the affected area can precede by an hour or two the development of small, closely grouped vesicles on a red base.
The recurrent outbreak lasts normally 7 days.
However rare, episodes of neuralgia in legs and buttocks and difficulty to urinate might occur. Such episodes, however, happen in a minor percentage of cases.
The most important factor in recurrent genital herpes is not the severity but the frequency of outbreaks. If outbreaks come once or twice a year there is a modest impact in the patient’s life.
If the number of outbreaks increases noticeably (one soon after the other), although not severe, they might affect the patient psychologically because his/hers social life will be disrupted.
Although the infection can stay in the body indefinitely, the number of outbreaks tends to decrease over a period of years
ASYMPTOMATIC VIRAL SHEDDING
Asymptomatic viral shedding can occur independent of outbreaks. It means that the HSV virus is in the mucous membrane even if there are no symptoms.
Asymptomatic viral shedding is well documented as the source of at least 70-80% of the cases of genital herpes transmission.
It virtually comes in all the patients infected with HSV-2. The shedding time cannot be predicted on the basis of age, sex or anamnesis.
It was believed that the virus didn’t spread between outbreaks, nowadays we know that it may also spread between outbreaks.
It is believed that 15-30% of men and 30-55% of women get infected between outbreaks. The shedding occurs in the mucous membranes of the genital area and most frequently in the periods preceding and succeeding the outbreak.
People infected with HSV- are most prone to the occurrence of shedding than those infected with HSV-1 and those who have frequent outbreaks.
However the incidence of asymptomatic shedding is greatest during the first year or two after infection, transmission potentially occurs even after.
Herpes serology test is extremely important for the correct information to patients and partners and gives the possibility to minimize contagion through anti viral treatment.
BEHAVIOUR
While it is impossible to know when and where will occur, we surely know who is going to have it. Counseling of infected persons and their sex partners is critical to management of genital herpes.
It is fundamental that the infected person:
-
Informs the sexual partner
-
Is aware of outbreaks and avoids sexual activity
-
Uses condoms for any kind of sexual activit
REMEMBER
Symptomatic Recurrence Symptoms are:
Itching, burning or tingling in the affected area
can precede the outbreak by an hour or two, to the development of small, closely
grouped blisters on a red base
The blisters burst, leaving painful ulcers that dry, scab and heal in approximately 72 – 96 hours. Scars will disappear within 4-12 days.
ATTENTION! EXTREMELY HIGH RISK OF TRANSMISSION
The blisters burst, leaving painful ulcers that dry, scab and heal in approximately 72 – 96 hours. Scars will disappear within 4-12 days.
FOR A SAFER SEX
-
Remember that genital herpes can be transmitted not only through genital to genital, oral and anal sex, but also though contact with the infected area without penetration. Whenever there is a skin to skin contact, there is a potential risk.
-
Use condom during any sexual contact
RISK FACTORS
-
Females:women are more at risk than men because of the large genital mucous area exposed to the sexual contact, have greater chance to get infected than men.
-
Age: the infection risk increases with age.
-
Duration of sexual relationships:the longer the relationship with an infected person, the higher the chance to be infected.
-
Number of sexual partners: a high number of sexual partners increases the possibility of infection.
-
Years of active sexual life: in relation to higher sexual life expectancy and number of partners.
-
Frequency of sexual intercourses: an intense sexual life increases the risk of contracting herpes. The higher the number of relationships, the highest the risk of contracting herpes because at the beginning of a relationship sex is often more frequent than in long terms relationships.
-
Partners recently affected: those who have recently contracted herpes have a higher potential transmission risk because of higher occurrence of asymptomatic shedding.
Sexual orientation:
-
Male homosexuals are more at risk to contract HSV-2 infection than male and female heterosexuals.
-
Female homosexuals are at a lower risk to contract HSV- 2 than heterosexual male and female and male homosexuals.
-
Bisexual: a female homosexual having sex with a bisexual female has higher risk to get infected than having sex with an homosexual partner.
IMPORTANCE
OF DIAGNOSIS
IN GENITAL HERPES
From what previously stated becomes clear the importance of information.
This is the reason why we shall summarize herein under why comprehensive information will make people aware of the problem and therefore more prone to a correct behavior.
BECAUSE
-
Transmission risk diminishes if people are aware to be infected.
-
Patients know that they have to stop sexual activity during recurrences.
-
Patients can undertake medical treatment which reduces recurrences, asymptomatic shedding and transmission to others.
-
Patients know that they have to use condoms
-
Patients know that they have to inform their sexual partners.
-
Patients can know that they are infected through a blood test.
IF YOU KNOW IT,
YOU CAN DEFEND YOURSELF
THERAPIES
Prior to any kind of pharmaceutical prescription it is fundamental:
-
a diagnosis
-
give enough information regarding contagion, history and risk of transmission of the infection
Being herpes an easily mistaken disease, it is fundamental to know if it is:
-
a primary infection, recurrent episode or asymptomatic shedding
-
the patient’s immune system status
The treatment will be personalized accordingly.
The purpose of therapy is to:
-
cure symptoms;
-
prevent recurrent outbreaks;
-
prevent the transmission;
-
prevent the transmission to the baby in case of pregnancy.
Therapy consists of topic and systemic treatment, based on molecules such as aciclovir, famciclovir, valaciclovir. The prescription criteria is based on:
-
how soon the patient seeks for treatment;
-
intensity and localization of the episode;
-
frequency of outbreaks;
Sexual partners infected with HSV will have the same treatment.
In the case of partners not having symptoms, an accurate anamnesis on eventual previous genital lesions is recommended, as well as to give correct information on how herpes occurs and the possibility to have a blood test able to detect the virus
GLOSSARY
A - E
Antibody Protein produced by our body in response to particles extraneous to our body, as microorganisms and toxins. Antibodies travel in the blood, attack the particle and destroy it.
Antiviral A drug that fights and destroys viruses, or makes them unable to reproduce. Against HSV there are valacyclovir and famcyclovir.
Asymptomatic No evident signs of disease
Cervix The lower section of the uterus which protrudes into the vagina.
Episodic therapy Therapy of the herpetic infection which helps to relieve symptoms and to shorten the duration of outbreaks. It has to be taken at each outbreak.
F – I
First episode, of genital herpes First clinical episode in a subject never infected with the HSV virus before. This might be the most severe episode because the body hasn’t developed antibodies (defenses)
Human Immunodeficiency virus Virus of immunodeficiency
HSV Herpes Simplex Virus, the virus that causes genital and oral herpes. There are to types of HSV: HSV-1 and HSV-2, that most commonly causes genital herpes and HSV-1 that commonly causes oral herpes, but can also cause genital herpes.
Ganglia Groups of nerve cells in our organism.
Genital area The area where there are the reproductive organs: penis, testicles, vagina, vulva.
HIV Human Immunodeficiency virus
L – O
Latent Present, but inactive. Latent herpetic infection means that the virus is hidden in the body with no symptoms. HSV is present in groups of nerve cells called ganglia.
Mucous, Membrane Linings of all the body cavities: e.g. vagina, anus, mouth, nose. These areas are particularly prone to be infected with herpetic viruses.
Neonatal, herpes When the baby is infected with the virus during delivery, or soon after birth.
Non primary, genital herpes. The first episode in a subject that has antibodies against HSV, different from those which created the first infection. E.g. a subject previously infected with HSV-1 has antibodies for HSV-1, but not for HSV-2.
P – R
Perianal Located around the anus
Primary genital herpes. First outbreak in a subject never infected with the HSV virus before. This might be the most serious outbreak because the body hasn’t yet developed antibodies.
Prodrome Symptoms such as burning, tingling, indicating the development of the episode.
S – T
Sacral Near to the bottom of the spinal cord.
Sacral ganglia Groups of nerves close to the bottom of the spinal cord. HSV is latent (non active) in the sacral ganglia of an affected subject.
Sexually transmitted, disease Any disease that can be transmitted by sexual contact (e.g. syphilis, gonorreha, condilloms, HIV).
Serology Blood test that measures antibodies.
Suppressive, therapy. Daily therapy that helps to prevent, or reduce the frequency of outbreaks.
Transmission When the infection is transmitted from one to another person.
U – Z
Vesicul Little skin blister containing transparent liquid.
Virus Small part of material (DNA or RNA) enveloped in a protective shell that replicates itself only within cells of living hosts

