PAINFUL BRUISING SYNDROME
Luciano Schiazza M.D.
Dermatologist
c/o InMedica - Centro Medico Polispecialistico
Largo XII Ottobre 62
cell 335.655.97.70 - office 010 5701818
www.lucianoschiazza.it
Painful bruising syndrome (PBS), also called autoerythrocyte sensitization, is a painful purpuric condition that mainly occurs in white young to middle-aged females, nearly always emotionally-labile disturbed, without antecedent definited trauma or after insufficient trauma.
It was first described by Frank Gardner and Louis Diamond in 1955 (Gardner-Diamond syndrome). They describe “the occurrence, in four adult women, of an abnormal response to bruising, characterized by local pain, swelling and extension of bleeding into adjacent areas, often to a serious extent”. In 1961, Oscar Ratnoff and Agle observed tha most such patients had an undrlying psychiatric interface (psychogenic purpura).
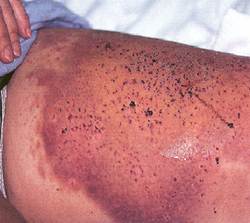
PBS is characterized by recurrent crops of ecchimoses commonly located over the extremities (arms and legs) and/or the face, heralded by a burning or stinging sensation. Bruising occurs after a day or so. The lesions appear suddenly as areas of redness progressing in ecchymoses.

They are non pruritic and disappeare in a week or so leaving a bruise-like discolouration.
PBS is due to allergic sensitivity to a component of the red cells (erythrocyte) membrane (phosphoglyceride) in the tissues: minor extravasation of blood is followed by severe inflammatory reaction.
Skin biopsy reveals dermal extravasation of RBCs along with haemosiderin around blood vessels surrounded by a lymphohistiocytic infiltrate, with no evidence of vascular lesion.
All routine haematological investigations are normal as the coagulation profile and the neurological investigation. Psichiatric evaluation can reveal multiple stressors in the patient’s day-to-day life or concomitant psychologic illness.
Intradermal sensitivity test is performed to confirm the diagnosis: patient’s own blood as a source of RBCs was taken and injected (0.1 ml) into the skin (forearm or intrascapular region) with a saline control on the opposite site. After 24 to 48 hours, in case of PBS, a painful rounded ecchymosis is seen at the site of injection, similar to those which appear spontaneously, without any reaction at the control site.
The differential diagnosis is with:
-
Von Willebrand’s disease,
-
vitamin C deficiency,
-
small vessel vasculitis,
-
anti-phospholipid syndrome,
-
drugs intake (ectasy use, ASA, NSAIDS, SSRIs, systemic glucocorticoids)
-
Ehlers-Danlos
-
Hereditary hemorragic teleangiectasia
-
Henoch-Schonlein purpura
So, when has diagnosis of PBS to be considered? In case of
-
recurrent painful ecchymoses
-
normal haematological evaluation as for the coagulation system
-
psychiatric comorbidities
There is no specific treatment for PBA. Plasmapheresis, oral cyproheptadine, psichotherapy has been tried.
